Peritoneal Dialysis and Its Associated Complications
November 22, 2021
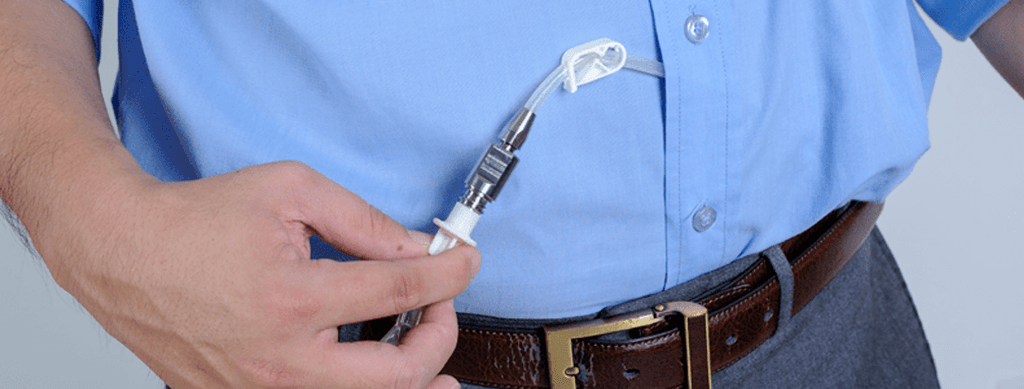
Worldwide, the number of patients suffering from chronic kidney disease (CKD) or loss of kidney function is gradually increasing. Due to this trend, the number of people who need renal replacement therapy is also on the rise. One of the major tasks of the kidneys is filtering the metabolites from the blood. If the kidneys can no longer perform this job, the blood must be cleansed and drained artificially through Dialysis (blood washing). Some patients choose the flexible method of Dialysis called peritoneal Dialysis (PD), which uses the peritoneum membrane as a filter. The advantage of peritoneal Dialysis is the flexibility it offers. It can be performed independently at home, significantly improving quality of life. In addition, this vascular-sparing form of removing excess water and dissolved urinary substances can better preserve any remaining kidney function. The solution used during PD is a mixture of salt, minerals, and dextrose (sugar) dissolved in water, called dialysis solution, and is placed in a person’s abdominal cavity through a catheter.
Peritoneal Dialysis-related infections, including peritonitis, exit‐site infections (ESI), and tunnel infections, are some of the complications resulting in significant morbidity and risk of death.
Early complications related to peritoneal access are divided into mechanical (bleeding, visceral perforation, dialysate leaks, catheter dysfunction, hernia formation, cuff extrusion) and infectious (early peritonitis, surgical wound, tunnel, and exit site infections).
Common Complications of Peritoneal Dialysis
- The most significant and commonly reported complication of peritoneal dialysis (PD) catheters is an infection called Peritonitis. It is an infection of the abdominal cavity’s lining (peritoneum). This infection can also develop where the tube (catheter) is inserted into the body to carry the cleansing fluid into and out of your belly.
- Weight gain. The dialysate contains sugar (dextrose). Absorbing some dialysates might even cause you to take in hundreds of extra calories daily. This can easily lead to weight gain. The extra calories you are getting can also cause high blood sugar, especially for those with diabetes.
- Holding fluid in your abdomen for extended time periods may even strain your muscles.
- Inadequate Dialysis. Peritoneal Dialysis can become ineffective after several years. You might need to switch to hemodialysis.
Protocols are in place to decrease the infection risk in PD patients and prevent complications of peritoneal dialysis. These include proper catheter placement, exit-site care including Staphylococcus aureus prophylaxis, careful training of patients with periodic re-training, prevention of contamination, and prevention of procedure-related and fungal peritonitis
Review
Dr. Umair Haider

